The intersection of bariatric surgery, fertility, and pregnancy presents unique challenges and opportunities. Bariatric surgery can lead to significant weight loss, which may improve fertility and reduce pregnancy related complications such as macrosomia and gestational diabetes – but it must be done with careful GP oversight.
Laparoscopic and bariatric surgeon Dr Jason Winnett (Winnett Specialist Group, Melbourne) shares answers to common questions about obesity and bariatric surgery in the reproductive years.
Infertility in the modern context: rising age and obesity
“The average of first baby back in 1961 was 23 years-old and today the average first childbirth for women is 30 years,” *1 says Dr Winnett.
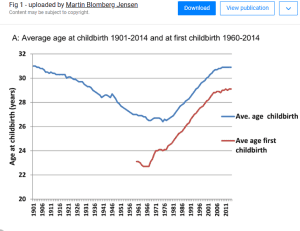
“37% of Australian women now have their first child between 30 and 37, a period where fertility rates decline significantly.
“Throw obesity and anovulation into the mix and it’s a double whammy.” According to one study of more than 600 women in Epidemiology, women with a BMI of more than 27 were three times more likely to be infertile. *2
“The good news is that ‘getting fit for fertility,’ which often includes bariatric surgery in this group, can greatly improve the chances of conception. One study from the American Society of Reproductive Medicine found that women who lost 10% of their body weight increased conception rates from 54% to 88%.”
How long should patients wait to try to fall pregnant after bariatric surgery?
“Most weight loss surgeons and GPs would advise waiting 12 to 18 months before trying to conceive after bariatric surgery,” says Dr Winnett. But there is minimal evidence to support this; losing more weight first is obviously advantageous.
This gives patients time to reach a more stable weight, adjust to surgery, and avoid complications like Dumping Syndrome *4 (especially after producers such as Roux-en-Y gastric bypass).
Many patients become pregnant 3 months post bariatric surgery, and it is still perfectly safe.
What are the main considerations GPs should keep in mind for bariatric surgery and pregnancy?
From our experience, the following can be particularly helpful for GPs during this period:
- Pre-eclampsia risk: consider low-dose aspirin for prevention in appropriate patients.
- Accurate blood pressure measurement: always use the correctly sized cuff.
- Nutritional monitoring: B12, iron and folate require close tracking, as deficiencies are common. The Australian Journal of General Practice provides clear protocols for managing anaemia and micronutrients in pregnancy.
- Close follow-up: Monitor women closely in the first year postpartum.
- Multidisciplinary input: encourage patients to work with a dietitian for tailored nutrition advice and pregnancy planning.
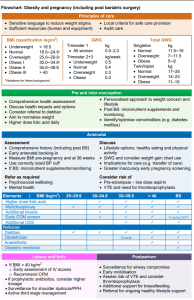
Source: Queensland Health Obesity and Pregnancy
Should I encourage patients to have surgery before baby or after pregnancy?
“Many women choose to do one or the other, however untreated obesity does increase the risk of common obstetric complications and also the risk of infertility,” says Dr Winnett.
According to a large study of 627,693 women published in the New England Journal of Medicine*5, women who had undergone bariatric surgery before pregnancy were compared with women of a similar BMI who had not had surgery.
- In the bariatric group, the rate of gestational diabetes was 1.9% compared with 6.8% in the non-surgery group.
- They were also less likely to have very large babies (8.6% vs 22.4%).
- Both groups had the same risk of congenital malformations.
There were, however, some downsides:
- The bariatric group had a slightly shorter average gestation (by about 4.5 days).
- The rate of stillbirth or neonatal death was 1.7% compared with 0.7% in controls. The study noted these events were rare and the difference was of borderline significance.
Dr Winnett explains: “It’s important to give patients the full data – to weigh the small but significant risks against the very real benefits of reduced gestational diabetes, macrosomia, and downstream health impacts on the child.”
Referral pathways: surgeon or fertility specialist?
The decision often comes down to timing and patient priorities.
- If pregnancy is planned for the near future (within the next 12 months), referral to a fertility specialist may be more appropriate.
- If pregnancy is planned further down the track (after at least 18 months), bariatric surgery can be considered first, with the option to involve infertility specialists later if needed.
When to Refer: updated BMI guidelines for Bariatric Surgery
- Patients with a BMI of 35 or higher, or BMI ≥35 with obesity related comorbidities (such as type 2 diabetes or high blood pressure)
- If a patient’s BMI does not meet these criteria, they may not qualify for the surgery.
- Consideration of the Body Roundness Index (BRI) in assessment
- Patients who are willing to engage in lifestyle change and psychological support
Patients not suitable for referral include:
- Patients with untreated or uncontrolled medical conditions such as heart, liver, or kidney disease, or blood clotting disorders, may not be suitable candidates for bariatric surgery because of the additional risks involved.
- Patients with a history of substance abuse, including alcohol or drugs, may not be suitable candidates due to the risk of not following post-surgery guidelines and a higher chance of complications.
- Patients who are planning pregnancy in the near future.
When to refer: Fertility specialist
Referral to a fertility specialist may be more appropriate for:
- Women with recurrent miscarriage or poor pregnancy outcomes
- Women over 35 who have not conceived after 12 months of unprotected intercourse
- Women over 36 who have not conceived after 6 months
- Patients with PCOS or endometriosis
Supporting Women Through Their Journey
Pregnancy after bariatric surgery is becoming increasingly common, and many women will look to their GP for advice along the way. Talking through timing, supporting nutrition, and linking in with specialist care can make the journey smoother for both mother and baby.
At Winnett Specialist Group, we focus on careful assessment, surgical treatment when appropriate, and ongoing post-operative support with our dietitians, psychologists, and exercise specialists. If you have patients considering surgery as part of their path to pregnancy, we’re here to work alongside you in their care.

Dr Jason Winnett
Laparoscopic and Bariatric Surgeon
P (03) 9417 1555 admin@winnettspecialistgroup.com.au
www.winnettspecialistgroup.com.au
Queens Terrace, 382 Victoria Parade, East Melbourne 3002
Sources:
1 Australia’s mothers and Babies, AIHW, 2025
2 Body Mass Index and Ovulatory Infertility, Epidemiology, 1994
4 Pregnancy following bariatric surgery management, Obesity Surgery 2016
5 Outcomes of pregnancy after Bariatric Surgery, NEJM, 2015
The Conversation, How Does Being Overweight Affect My Fertility?
National Demographic 2023, Does a woman’s fertility really plummet at age 35?